Thyroid Cancer

What is Thyroid Cancer?
Thyroid cancer occurs in the thyroid gland — a butterfly-shaped gland located at the front of the neck. This gland plays a critical role in regulating metabolism, heart rate, and body temperature by producing thyroid hormones. While most thyroid nodules are non-cancerous, some may develop into thyroid cancer.
Risk Factors for Thyroid Cancer
Several factors may increase your risk of developing thyroid cancer:
Age and Gender
More common in women; risk increases after age 50.
Genetic Conditions
Certain inherited syndromes, such as MEN 2, familial adenomatous polyposis, and Cowden syndrome.
Family History
Having first-degree relatives (parents, siblings, or children) with thyroid cancer.
Radiation Exposure
Exposure during childhood for conditions like lymphoma or neuroblastoma increases risk.
Low Iodine Intake
Linked to a higher chance of developing papillary and follicular thyroid cancers.

Symptoms of Thyroid Cancer
Thyroid cancer often develops silently, but some of the common signs and symptoms include:

Lump in the Neck

Throat Discomfort
Difficulty Swallowing

Hoarseness or Voice Changes

Breathlessness
Incidental Finding: Some thyroid cancers are detected accidentally during scans for unrelated health issues.
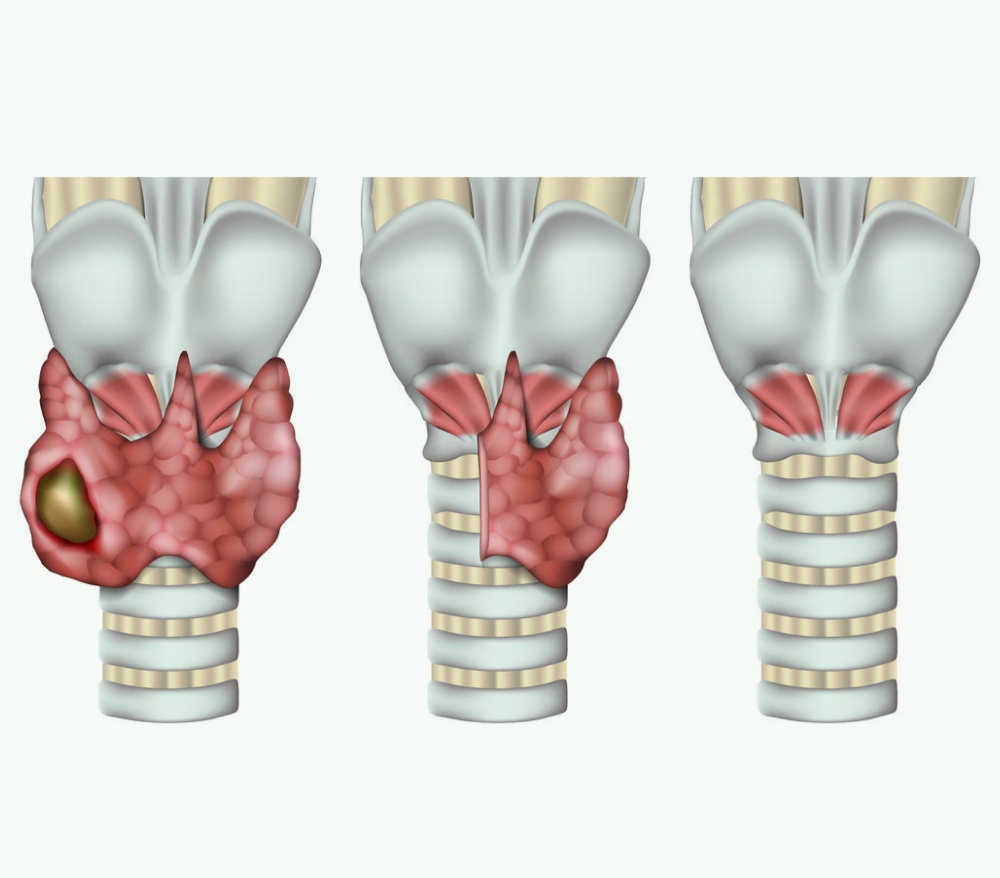
Types of Thyroid Cancer
Thyroid cancers are classified based on the type of cells involved and their behaviour:
- Differentiated Thyroid Cancer
The most common type, includes:
- Papillary carcinoma (most frequent)
- Follicular carcinoma
- Hürthle cell carcinoma
- Medullary Thyroid Carcinoma
Develops from C-cells in the thyroid and may be hereditary. Associated with MEN 2 syndrome.
- Anaplastic Thyroid Carcinoma
A rare but aggressive form of thyroid cancer that spreads rapidly and is difficult to treat.
How Thyroid Cancer Is Diagnosed
Clinical Examination
A detailed physical check of the neck to feel for lumps or irregularities.
Imaging Tests
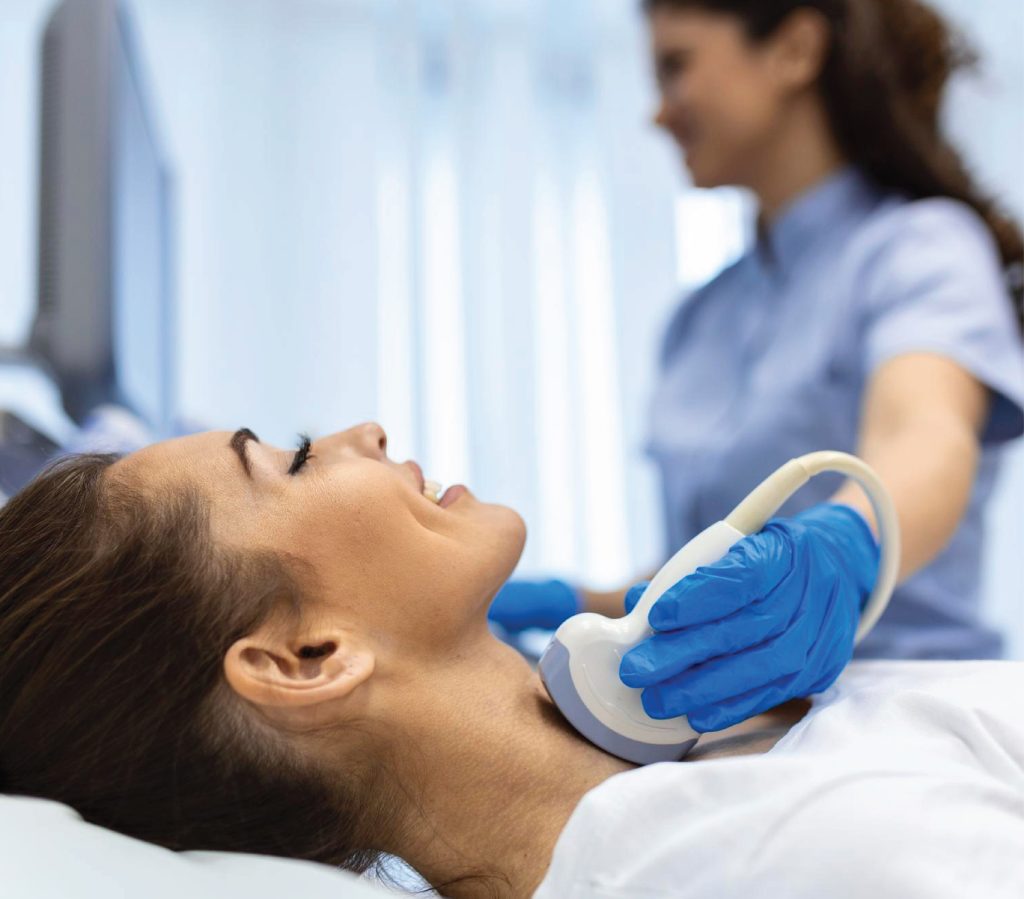
Neck Ultrasound:
First-line imaging to assess thyroid nodules. Results are often classified using the TIRADS system.
CT/MRI Scan:
Used for advanced disease or if the cancer extends beyond the thyroid.
PET-CT Scan:
Recommended if cancer is suspected to have spread to other parts of the body.
FNAC (Fine Needle Aspiration Cytology)
A minimally invasive procedure where a fine needle is used to extract cells from the thyroid lump for microscopic evaluation. FNAC under ultrasound guidance improves accuracy.
Blood Tests
Thyroid Function Tests: Help assess whether the thyroid is underactive or overactive.
Thyroglobulin Test: A tumour marker used especially in the follow-up of differentiated thyroid cancers.
Treatment Options for Thyroid Cancer
Treatment is based on the type and stage of cancer, and patient-specific factors. Most thyroid cancers are highly treatable.
Surgical removal is the cornerstone of thyroid cancer treatment. Options include:
- Lobectomy: Removal of one thyroid lobe.
- Total Thyroidectomy: Complete removal of the thyroid gland.
- Lymph Node Dissection: If cancer has spread to nearby lymph nodes.
Robotic thyroid surgery is now available and offers a minimally invasive alternative with better cosmetic results.
Used after surgery to destroy remaining cancerous thyroid tissue, especially in papillary and follicular thyroid cancers.
External beam radiation is rarely used but may be recommended in certain aggressive or unresectable cancers.
Thyroid cancer is generally resistant to chemotherapy. However, advanced or metastatic cases may benefit from:
- Targeted therapy (e.g., tyrosine kinase inhibitors)
- Immunotherapy for rare, treatment-resistant types



