Cervical CANCER

Cervical cancer care at Thangam cancer center
Cervical cancer occurs in the cervix, the lower part of the uterus that opens into the vagina. It is one of the most managable forms of cancer when detected early and managed appropriately. The primary cause of cervical cancer is a persistent infection with the Human Papillomavirus (HPV) — a common sexually transmitted virus.
At Thangam Hospital, we offer advanced cervical cancer screening, vaccination, and treatment, empowering women to take proactive control of their reproductive health.
What Causes Cervical Cancer?
While many HPV infections resolve on their own, a persistent high-risk HPV infection can lead to abnormal changes in cervical cells, which may develop into cancer over time.
Common risk factors associated with cervical cancer include:
Multiple sexual partners
- Increases exposure to HPV.
- Early onset of sexual activity
- Poor genital hygiene
History of sexually transmitted infections (STIs)
Including HIV, chlamydia, syphilis, or gonorrhea.
Weakened immune system
Due to autoimmune disorders or prolonged use of immunosuppressive medications.
Smoking
Tobacco exposure is linked to higher cervical cancer risk.
Hormonal fluctuations
Especially changes in progesterone levels.
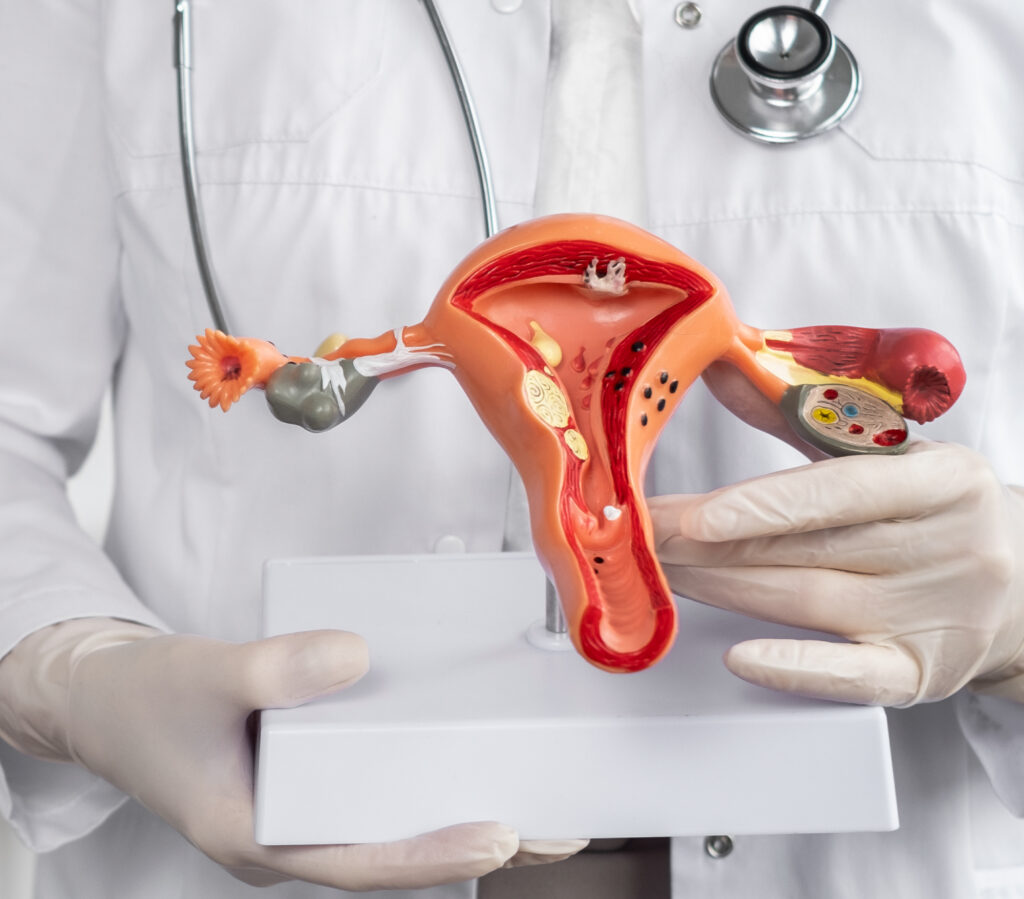
Symptoms of Cervical Cancer
Cervical cancer often presents no symptoms in the early stages, making routine screening even more critical.
When symptoms do appear, they may include:
Early symptoms:

Unusual vaginal bleeding (especially after intercourse or between periods)

Watery or foul-smelling vaginal discharge

Pelvic pain or discomfort during intercourse
Advanced symptoms (as cancer spreads):

Persistent pelvic or
lower back pain

Swelling in the legs

Pain or difficulty
during urination

Kidney complications or failure

Blood in urine or stools
Bone pain

Unexplained weight loss

Fatigue and vomiting
If you notice any of these signs, we recommend consulting a gynecologic oncologist
or visiting our women’s cancer care unit at the earliest.

HPV and Cervical Cancer Prevention
HPV vaccination is highly effective in preventing infection from the high-risk strains of the virus that cause most cervical cancers. It is recommended for teenagers and young adults, ideally before sexual debut.
Regular cervical screening (Pap smear or HPV testing) for sexually active women helps detect early cell changes, allowing for timely treatment before cancer develops.
Cervical Cancer Diagnosis and Management
At Thangam Cancer Center, our approach to cervical cancer diagnosis includes:
- Pap smear & HPV testing
- Colposcopy (visual examination of the cervix)
- Biopsy to confirm the presence of cancerous or precancerous cells
- Advanced imaging (MRI, CT, or PET-CT) to determine the stage and spread
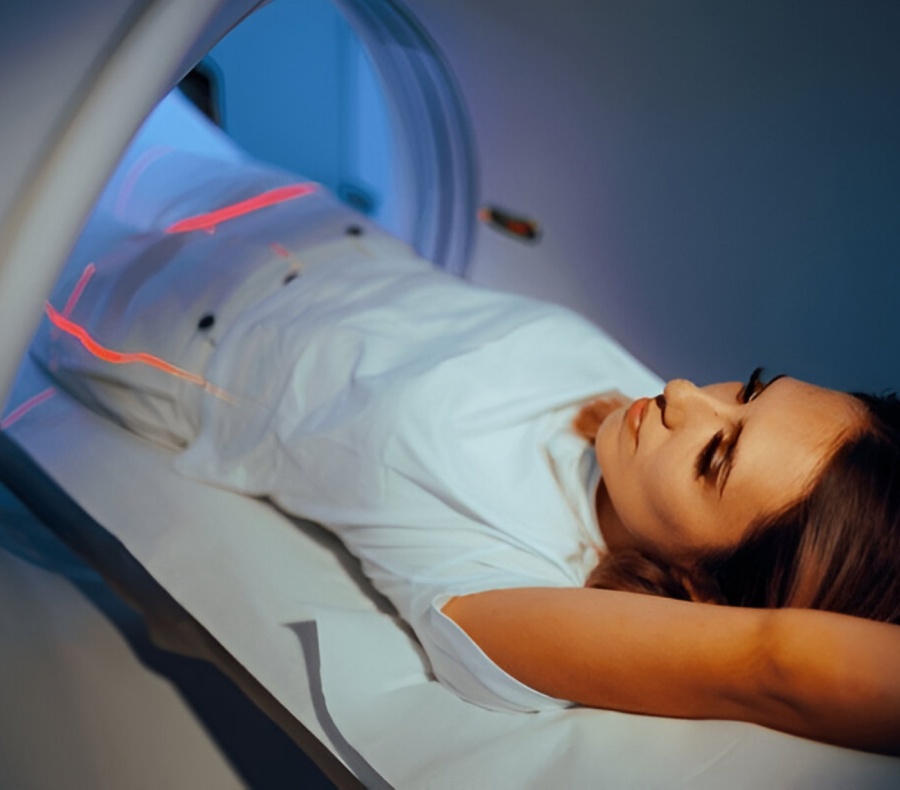
Treatment Options for Cervical Cancer
Treatment depends on the stage of cancer, age and overall health of the patient. Our multidisciplinary team designs a personalized treatment plan that may include:
- Patients with precancerous lesions undergo a minor surgical procedure called LEEP (Loop Electrosurgical Excision Procedure), where an electrically heated wire loop removes cells from the cervical region.
- If the tumour is relatively small, a fertility-sparing approach is preferred, and trachelectomy is performed.
- In more advanced cases, Radical hysterectomy is done with Lymph Node dissection. In elderly, postmenopausal patients, the ovaries are also removed.
- When the tumour is large or has spread beyond the uterus, radiation therapy with or without chemotherapy is used.
- High-energy X-rays target cancerous areas to destroy malignant cells and stop their growth.
- Radiation may be external or internal (brachytherapy) and affects only the treated area.
- In external beam radiation therapy, energy beams are directed at the pelvis using a Linear Accelerator with techniques like 3DCRT, IMRT, IGRT, or Rapid-Arc.
- Brachytherapy is a boost therapy which is delivered special applicators.
- Palliative radiotherapy is used in advanced stages when cancer spreads to organs like the liver, bones, or brain, to relieve symptoms such as bleeding, bone pain, or CNS issues
- In chemotherapy, oral medications are used to eliminate cancer cells; the intensive treatment is continuously given in cycles (usually weekly) with a short recovery period in-between.
- In metastatic cancers where the tumours have spread beyond the local region, chemotherapy is given as a palliative treatment.
- Uses drugs that specifically target cancer-related genes and proteins that help cancer cells grow and survive.
- This therapy aims to block the growth signals in cancer cells while minimizing damage to healthy tissue.
- Boosts the body’s natural immune system to help it recognize and attack cancer cells more effectively.
- This treatment is generally used in specific types of colorectal cancer that have identifiable genetic markers.






